- Email:info@psycare.it
- WhatsApp: +39 375 703 9065
20 Feb
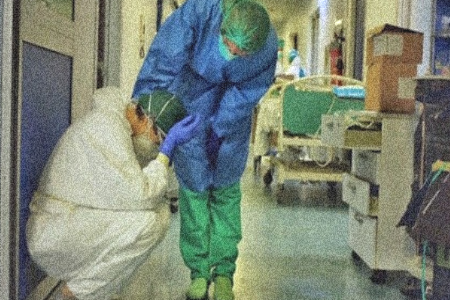
Healthcare workers and COVID-19 They are the antagonists in a story as dramatic as it is unreal. Unfortunately, it remains relevant today.
We say it without fear of contradiction: the health workers were crucial to the response to the pandemic COVID-19; and they still are. They face greater risks of infection than anyone else in carrying out their work; they are exposed to dangers such as psychological distress, fatigue, and stigma. Therefore, they are doubly victims.
Also apply for Nobel Peace Prize, on the proposal of the Gorbachev Foundation (which has its most characteristic activity in the organization of the World Summits of Nobel Peace Prize Winners), according to which the high merit should be recognized to “doctors, nurses, pharmacists, psychologists, physiotherapists, biologists, technicians, civil and military workers all, who
They faced the COVID 19 emergency in often dramatic and prohibitive situations with extraordinary self-denial, many of them sacrificing their own lives to preserve those of others and to contain the spread of the pandemic..
The new adversary: vicarious trauma
Beyond the pandemic, in fact, the vicarious trauma It is the second – but not secondary – opponent of the category. The literature describes vicarious trauma as a post-traumatic suffering, similar to the experiences of direct victims (Brady et al., 1999). Vicarious trauma is the phenomenon that derives from the empathic involvement between those who work in a helping profession and those who are actual victims of a first-hand trauma. Vicarious trauma is then joined by the burnout (Beck 2011; Ricard 2015), serious and drastic consequences of the poor quality of professional life in the helping professions; and leads to a total loss of interest in the people to whom the professional should direct his or her attention.
And these disorders, besides not being the only ones to manifest themselves, are often unavoidable if not treated promptly.
A valuable resource for the health workers , especially following the pandemic COVID-19, is definitely psychological support. To regain balance and serenity and protect one’s physical and mental well-being; also preventing burnout. The difficulty lies in not underestimating the problem.
2021 has been designated the International Year of Health and Care Workers (YHCW: Year of the Health and Care Workers). This is in appreciation and gratitude for the unwavering dedication of the health workers in the fight against the pandemic COVID-19.
And theOMS is launching a campaign highlighting the urgent need to invest in health workers. LOMS, in fact, is active in this sense towards a category as important as it is (often) renowned. In addition to providing advice on carrying out their duties, theOMS same provides, for the health workers, even the most recent guidance and training also in consideration of the pandemic from COVID-19.
So, that of the health workers This category of workers, due to the specific nature of their professional activity, is most likely to come into contact with potentially infected individuals. This is confirmed by data emerging from the ongoing epidemic. Protecting their health and safety is a key concern and is being monitored by all major international organizations. WHO, the European Centre for Disease Control (ECDC), INAIL (National Institute for Insurance against Accidents at Work), and the U.S. Centers for Disease Control and Prevention (CDC) issue continuously updated documents.
But in terms of mental health consequences, how are the men and women in healthcare workers doing?
Healthcare workers and industry research: the psychological impact is real
In a recent cross-sectional study conducted in China on health workers in several hospitals equipped with departments for patients with COVID-19 in several regions, a considerable percentage of health workers reported experiencing symptoms of depression, anxiety, insomnia, and distress, particularly women, nurses, especially those on the front lines and directly involved in the diagnosis, treatment, or provision of nursing care to patients with COVID-19 suspected or confirmed.
The psychosocial effects of quarantine in health workersFurthermore, they also affect the work environment, in addition, of course, to the personal sphere. Symptoms such as decreased work performance and a reluctance to continue working are common. They can also appear several years after the traumatic event. And, to this day, the pandemic is still ongoing.
These results suggest, therefore, that the health workers exposed to COVID-19, especially on the front lines, are at high risk of developing adverse mental health outcomes and may need psychological support.
It is clear to everyone how, health workers and those engaged on the front lines in dealing with the pandemic COVID-19 in various health service settings, are exposed to emotional overload in addition to the risk of infection.
Even in peacetime, the scientific literature on work-related stress has largely confirmed what has emerged in recent years. The healthcare sector is inherently characterized by the presence of psychosocial risk factors; emergency situations, daily exposure to extreme suffering, and potential additional risks. Therefore, the literature also shows interest in this aspect of the pandemic and seeks to manage its impact. COVID-19 on the psychological and emotional sphere of health workers on the front line. International support programs such as those shared by the MDPI (Multidisciplinary Digital Publishing Institute) e articles on the promotion of mental health in the health sector from European Agency for Safety and Healt at Work.
The first step, the first support for the profession, comes from acknowledging the evidence. The existence of factors that inevitably change the game, even for those who do this professionally; factors that increase the risk of burnout. This burnout, better known as burnout, particularly affects those who care for suffering people on a daily basis. This is without underestimating the other factors that intervene and impact the psychosocial consequences of a viral pandemic.
Social isolation also affects healthcare workers
The health workers who responded to the spread of COVID-19 reported high rates of symptoms of depression, anxiety, insomnia, and distress. Therefore, the protection of health workers is an important component of public health measures to address the epidemic of COVID-19 still ongoing. Special interventions to promote mental well-being in health workers exposed to COVID-19 should be promptly implemented.
During an epidemic, the health workers They are constantly exposed to extremely high levels of psychological stress, even when preventive and protective measures are deemed adequate. This ranges from the real fear of contracting the infection and transmitting it to family members, to prolonged separation from their families; without forgetting or underestimating the high mortality rate among healthcare workers. This confirms that it’s not just numbers, Amnesty International reports the death toll among the 17,000 health workers in this pandemic from COVID-19. And it dispels any doubts about the risk exposure they face and the psychological impact this pandemic is having on each of them.

Already in March last year, the WHO shared in an official document the recommendations to promote the management of stress associated with the global health emergency from COVID-19 with messages addressed directly to the health workers. The Inter-Agency Standing Committee (FISH) has released a briefing note; and summarises key considerations on mental health and psychosocial support (MHPSS) in relation to the COVID-19 pandemic. COVID-19. The document provides indications on the behaviors that healthcare personnel can adopt to prevent and reduce stress related to the particular situation they are facing..
Confirming how hot the topic still is, some psychological support networks supporting the health workers have already been set up. The same FNOPI (National Federation of Nursing Professional Orders) has launched fundraising initiatives to reimburse psychotherapy where necessary. The project #WeWithNurses of FNOPI, for nurses affected by the pandemic, in the psycho-physical care and rehabilitation paths is still active.
The problem, therefore, is far from solved. Although the issue is, today more than ever, deeply felt.
It should be emphasized, however, that these are temporary solutions, momentary responses to recurring problems. There has been a lack of real awareness of the issue, of the dramatic situation experienced daily by healthcare workers; a daily experience that has now lasted more than a year..
The data speaks clearly, too clearly: the health workers they also need this type of support above all. telemedicine It can also be a support for them. It would therefore be advisable to anticipate their needs and organize ourselves as best we can, both immediately and for the coming years..
When will there be evidence of the psychophysical impact that the pandemic has had? COVID-19 had on them, it will be too late to intervene. And this time we will be the ones who will have to run to their aid. Of course: as individuals and as workers..
Articoli Recenti
PsyCare
 The patient sees himself in the video consultation: when it is necessaryEdited By Josef
The patient sees himself in the video consultation: when it is necessaryEdited By Josef The digital signature in PsyCare? Just a click away!Edited By Josef
The digital signature in PsyCare? Just a click away!Edited By Josef Sharing a document online: it’s easy on PsyCareEdited By Josef
Sharing a document online: it’s easy on PsyCareEdited By Josef PsyCare’s online calendar reminds you of appointments with a reminder!Edited By Josef
PsyCare’s online calendar reminds you of appointments with a reminder!Edited By Josef Personalizing your online session invitation: why it’s importantEdited By Josef
Personalizing your online session invitation: why it’s importantEdited By Josef Patient ID: Is it mandatory?Edited By Josef
Patient ID: Is it mandatory?Edited By Josef Online group therapy? You can do it on PsyCare!Edited By Josef
Online group therapy? You can do it on PsyCare!Edited By Josef Drawing, shapes, and images in psychotherapy: online with the virtual whiteboardEdited By Josef
Drawing, shapes, and images in psychotherapy: online with the virtual whiteboardEdited By Josef
GDPR and Regulations for Psychologists
WhatsApp: +39 375 703 9065
General Inquiries: info@psycare.it
Support: help@psycare.it
Follow Us
Support
Initiatives

PsyCare for the Environment
We offset CO₂ emissions by planting a tree for every activated subscription: learn more.